OPD :(Out Patient Department )
1. Common an Age-Related Eye Illnesses
- Cataracts: A clouding lens of the eye that can basis blurred vision.
- Glaucoma: By the eye illness it harms the optic nerve which leading to visualization lost.
- Age-Related Macular Deterioration (AMD): A condition that disturbs the middle portion of the eye, foremost to defeat of dominant visualization.
- Diabetic Retinopathy: An impediment of diabetes which harm the blood vessels in cornea.
- Other Age-Related Vision Problems
- Presbyopia: A gradual loss of near vision that often begins in middle age.
- Dry Eye Disorder: An ailment caused by inadequate tear manufacture or poor tear eminence.
- Floaters: Miniature spots or specks that seem to float in your arena of vision.
- Eye Care Professionals
To address these eye situations, it’s significant to seek the expertise of qualified vision care professionals. These include
- Ophthalmologists: Medical doctors who specialise in eye health and surgery.
- Optometrists: Healthcare professionals who provide primary eye care, including vision exams and the prescription of eyeglasses and contact lenses.
- Opticians: Professionals who make, dispense spectacles and lenses.
- Vision Tests and Corrective Lenses
A comprehensive eye exam is essential for detecting and managing eye conditions. In an eye examination, it care professional will use several tests, including the Snellen chart, to assess visual acuity.
Curative lenses, such as eyeglasses and lenses, can support correct refractive faults like:
- Myopia: The near-sightedness, struggle seeing distant substances.
- Hyperopia: The farsightedness, trouble seeing close substances.
- Astigmatism: A condition that causes blurred visualization at all distances owing to an irregularly formed cornea.
1.4.2 CATARACTS
Cataracts, a blurring of the eye’s lens, are an equal age-related eye illness. While they often develop gradually, various factors can contribute to their formation.
- Underlying Causes
- Oxidative Stress: Exposure to oxidative stress, caused by factors like ultraviolet radiation and pollution, can damage the lens proteins, leading to cataract formation.
- Age-Related Changes: As an age was arising, the proteins in an eye’s lens can mass together, triggering the lens to become gloomy.
- Medical Circumstances: Circumstances, like as diabetes, can upsurge the hazard of emerging cataracts.
- Medications: Long-term habit of corticosteroids and extra medications can donate to cataract formation.
- Trauma: Eye injuries can harm the lens and upsurge the hazard of cataracts.
- Radiation Exposure: Exposure to radiation, such as from X-rays or radiation therapy, can also increase the risk.
- Risk Factors
Several causes can upsurge the risk of emergent cataracts, containing
- Age: The risk of cataracts increases with age.
- Smoking: A smoking is a substantial risk issue for cataracts.
- Extreme Alcohol Consumption: The over consumption of alcohol can also upsurge the risk.
- Obesity: Being overweight or obese can contribute to cataract formation.
- High – Blood Pressure: It can damage the blood vessels of eye and increasing the harm of cataracts.
- Family History: A family antiquity of cataracts can upsurge your hazard.
- Exposure to UV Contamination: Excessive acquaintance to ultraviolet radiation from the sun can harm the lens.
1.4.3 GLAUCOMA
It is a risky eye illness which can prime to irretrievable visualization damage if remain crude. It is characterised by harm to the ophthalmic nerve, the nerve that links the eye to the brain.
The protagonist of Intraocular Pressure
A main factor in glaucoma development is elevated Intraocular Pressure (IOP). This compression is instigated by a build-up of liquefied within the eye. Usually, these fluid sanitations out of the eye over a drainage channel. However, if this channel becomes blocked or dysfunctional, the compression in the eye can upsurge, damaging the ocular nerve.
Types of Glaucoma
There are various categories of glaucoma, including:
- Open Angle Glaucoma: The utmost general type, it often progresses slowly without noticeable symptoms.
- Angle Closure Glaucoma: A fewer but more severe category, it happens when the drainage approach, where the iris meets the cornea, becomes narrow, blocking fluid flow.
- Normal Tension Glaucoma: This type happens when the ocular nerve harm happens despite normal eye pressure.
Risk Aspects for Glaucoma
Several aspects can upsurge your risk of rising glaucoma:
- Age: The hazard of glaucoma upsurges with age, specifically after age 40.
- Family History: A family antiquity of glaucoma can upsurge your hazard.
- Eye Injuries: Past eye injuries can damage the delicate structures of the eye.
- Certain Medications: The long-term practice of corticosteroids can upsurge eye pressure.
- Medical Circumstances: Circumstances like diabetes and high blood pressure can developed to glaucoma.
- Ethnicity: People of African, American, Hispanic, and Asian ancestry have a complex risk of developing glaucoma.
Early Detection and Treatment
Initial detection and treatment are critical for handling glaucoma. Regular eye exams are essential, especially for individuals at high risk. If glaucoma is diagnosed, treatment options whitethorn includes:
- Eye Drops: The Medications to lower eye compression.
- Laser Treatment: A minimally invasive procedure to improve fluid drainage.
● Surgery: In unadorned cases, surgery may be required to create a new drainage channel.
1.4.4 KERATOCONUS: A Progressive Eye Condition
Chart: 1.01 KERATOCONUS: A Progressive Eye Condition
Source: https://images.app.goo.gl/jLKWQ4Dyd1zpGe8q6
Keratoconus is a progressive eye ailment that reasons the cornea, it clear front layer of the eye, to reedy and bulge outward into a cone-like form. This irregular shape of cornea can lead to substantial vision problems, as well as blurred visualization, sensitivity to light, & difficulty with night vision.
Causes of Keratoconus
While the meticulous reason of keratoconus is unidentified, it is whispered to be a genetic form. It often affects both eyes, although one eye may be more severely affected than the other.
Symptoms of Keratoconus
The symptoms of keratoconus typically begin to appear through puberty or initial adulthood. These indications may comprise:
- Blurred visualization
- Sensitivity to light
- Struggle to driving at night
- Common changes in eyeglass or contact lens prescription
- Distorted vision
Treatment Options
The treatment for keratoconus depends on the strictness of the condition. In the early stages, eyeglasses or lenses may be sufficient to correct visualization. However, as the condition progresses, more advanced treatment options may be necessary, including:
- Corneal Cross-Linking (CXL): A non-surgical procedure that strengthens the cornea and slows down the development of the illness.
- Corneal Implants: Small, lens-like devices that can be rooted into the cornea to progress visualization.
- Corneal Transplant: In simple cases, a corneal transplant may be required to swap the harm cornea with a vigorous donor cornea.
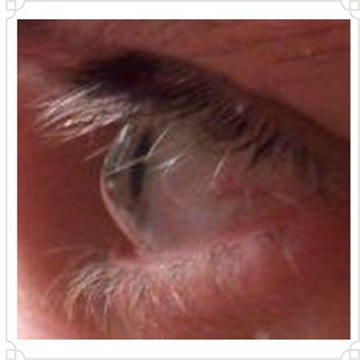
1.4.5 LOW VISION: A Diminished Ability to See

Source: https://www.gomabainetralaya.org/Lowvision
Low vision denotes to a visual diminishing that cannot be modified with standard eyeglasses, or lenses, or medical or clinical intervention. While it doesn’t necessarily mean complete blindness, it significantly impacts a person’s skill to accomplish regular tasks and activities.
The Reasons of Low Vision
Numerous conditions can represent to low visualization, including:
- An Age – Related Eye Diseases:
○ An Age-related macular degeneration (AMD)
○ A Cataracts
○ A Glaucoma
- An Eye Injuries
- etinal Diseases:
○ Diabetic retinopathy
○ Retinitis pigmentosa
- Neurological Disorders:
○ Stroke
○ Brain injury
- Congenital Conditions:
○ Albinism
○ Congenital cataracts
mpact of Low Vision
Low vision can affect a person’s quality of life in various ways, including:
- Difficulty with daily activities: Reading, writing, driving, and using electronic devices can become challenging.
- Social isolation: Visual impairment can represent to social separation and abridged contribution in social happenings.
- Emotional distress: Low vision can cause feelings of frustration, anxiety, and depression.
Managing Low Vision
While there’s no cure for low vision, several strategies can support individuals accomplish their condition and progress their eminence of life:
- ow Vision Rehabilitation: Specialised training to help individuals adapt to their vision loss and learn techniques to maximise their remaining vision.
- Assistive Devices: Magnifiers, reading glasses, and electronic devices with text-to- speech capabilities can aid in daily tasks.
- Lighting: Proper lighting can improve visual clarity and reduce eye strain.
- An Eye Exercises: Consistent eye exercises can increase strengthen eye muscles and progress visual function.
By sympathetic the reasons and impact of low vision, individuals can take the steps to manage their condition and live fulfilling lives.

1.4.6 DIPLOPIA: The Perception of Double Vision
Chart: 1.03 DIPLOPIA: The Perception of Double Vision
Source:https://www.medicalnewstoday.com/articles/170634#definition
Diplopia, also recognized as double image, is a visual illness where a specific perceives two images of a single object. This can be a troubling and disorienting experience that disrupts daily activities.
Symptoms of Diplopia
Diplopia can be accompanied by various additional symptoms, including:
- Misalignment of the Eyes: One or both eyes may not be aligned properly, causing a
“wandering eye” or “cross-eyed” appearance.
- Eye Pain: Pain may be experienced when moving the eyes.
- Facial Pain: Pain may be felt around the eyes, in the temples or eyebrows.
- Headache: Headaches can be a common occurrence with diplopia.
- Nausea: Double vision can sometimes induce nausea.
- Muscle Weakness: Weakness in the eyes or other parts of the body can be a symptom.
- Drooping Eyelids: Ptosis, or drooping of the upper eyelid, may be present.
1.4.7 Strabismus (Squint)
Strabismus, or squint, is a form where the eyes do not line up properly, reasoning them to point in dissimilar directions. This misalignment can lead to several vision glitches, including double image and reduced deepness perception.
Common Causes of Strabismus
- Muscle Imbalance: Frail or overactive eye muscles can reason the eyes to misalign.
- Neurological Disorders: Conditions affecting the nerves that control eye movement can contribute to strabismus.
- Refractive Errors: Substantial modifications in the refractive power of the two eyes can reason the eyes to turn inside or outside.
- Congenital Factors: A strabismus can be present at birth or develop early in childhood.
Risk Factors for Strabismus
- Family History: A family antiquity of strabismus can upsurge the hazard.
- Premature Birth: Premature babies are at higher risk.
- Certain Medical Conditions: Conditions like cerebral palsy or Down syndrome can be associated with strabismus.
Impact of Strabismus
If leftward uncured, strabismus can represent to:
- An amblyopia (Lazy Eye): The brain may suppress vision in the askew eye to avoid double vision.
- Reduced Vision: Decreased visual acuity and depth perception.
- Social and Psychological Issues: Strabismus can affect a person’s self-esteem and social interactions.
Cure for Strabismus
Cure for strabismus be contingent on the underlying cause and harshness of the condition. It may implicate:
- Eyeglasses or Lenses: It helps to make easy to identify.
- Eye Exercises: To fortify eye muscles and progress coordination.
- Patching: Casing the stronger eye to inspire the weaker eye to develop.
- Surgery: To regulate the eye muscles and progress alignment.